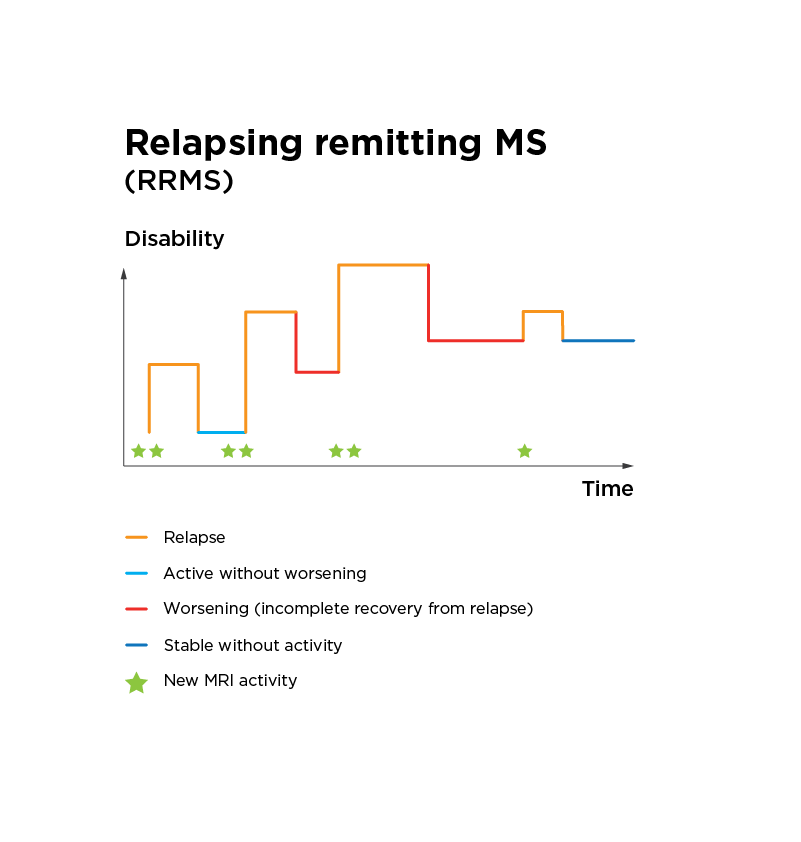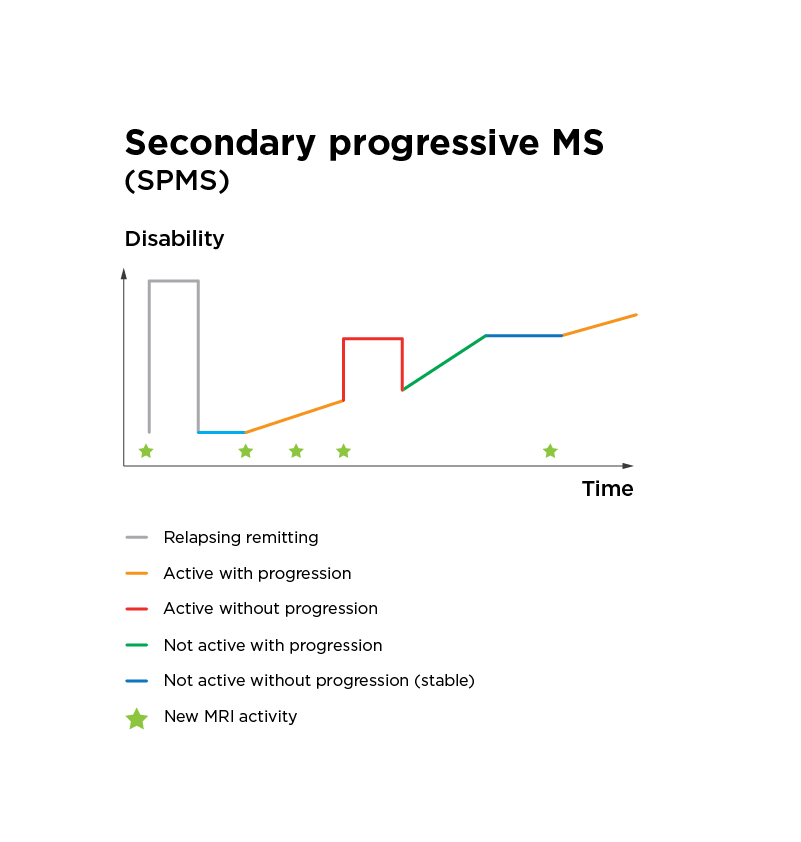Multiple sclerosis overview
The term multiple sclerosis means ‘many scars’ and refers to the damage caused to the nerve impulses within the brain, spinal cord and optic nerves. It is a highly variable condition and the symptoms of multiple scleroris depend on which areas of the central nervous system have been affected and where the scarring has occurred. There is no set pattern to MS and everyone with MS has a different set of symptoms, which vary from time to time and can change in severity and duration – even in the same person.
Living with multiple sclerosis
Over 33,000 people in Australia are living with multiple sclerosis, including 5,535 Queenslanders, and it affects each person differently. On average more than 10 Australians are diagnosed with MS every week. There is currently no known cure for MS however there are FDA-approved medication that have been shown to “modify” or slow down the underlying course of MS. In addition, many therapeutic and technological advances are helping people manage symptoms. Advances in treating and understanding MS are made every year, and progress in research to find a cure is very encouraging.
There is no known single cause of MS but many genetic and environmental factors have been shown to contribute to its development.
The current hypothesis is that the disease appears in those individuals who have a genetic predisposition to react to some infectious agents such as a virus or bacterium.
While several different viruses and bacteria have been studied for their possible role in MS, the trigger(s) have not yet been found. Environmental and psychological factors may play a part that we do not yet understand. We do know, however, that MS is not a contagious disease and you do not need to be concerned about transmitting MS to those around you.
Wrongly programmed immune cells enter the CNS, causing inflammation in the brain, spinal cord, and/or optic nerves. It is this inflammation that can cause damage to the protective myelin coating around the nerve cells, producing scars (also called plaques or lesions) that interfere with nerve transmission. While many of these scars may have no apparent effect, others are responsible for the various symptoms of MS.
There 3 most common ‘types’ of MS are:
- Relapsing remitting MS is the most common form of MS. It is characterised by flare-ups of the neurological symptoms of MS, also known as relapses or attacks, followed by periods of recovery or remission.
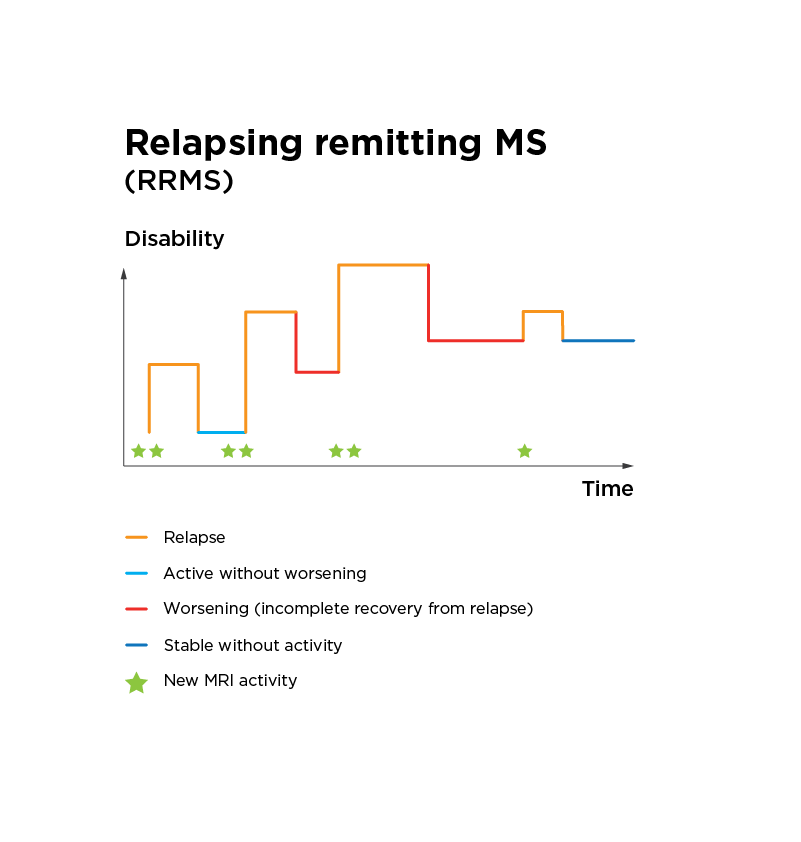
- Secondary progressive MS (SPMS) is a secondary phase of relapsing remitting MS that can develop years, to decades following the initial onset of relapsing symptoms. SPMS is characterised by a progressive worsening of symptoms (accumulation of disability) over time, with no obvious signs of remission.
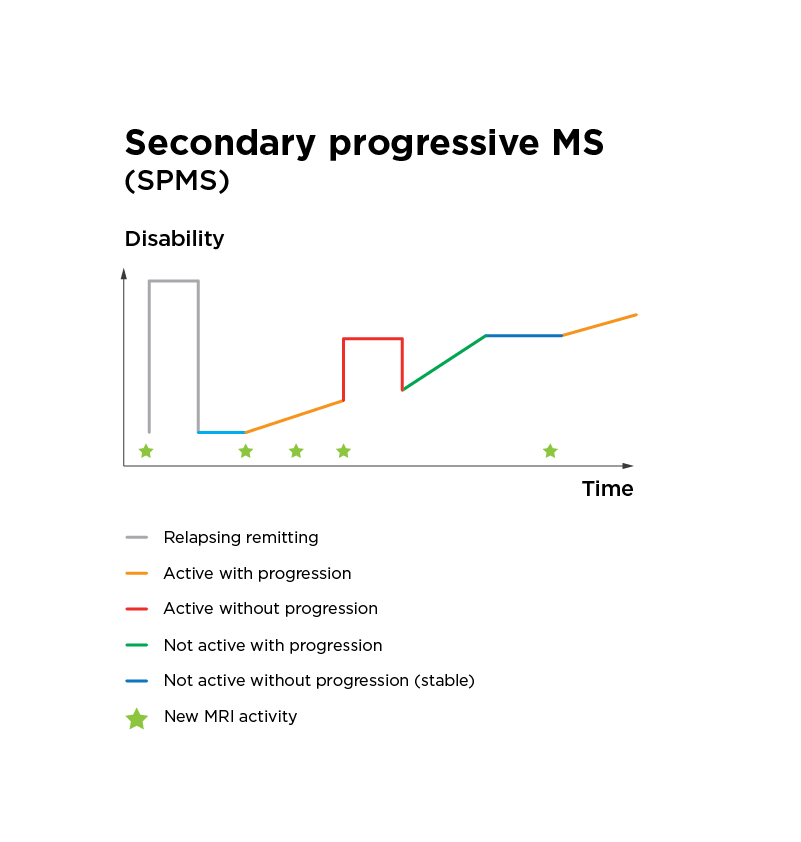
- Primary progressive MS (PPMS) is diagnosed in approximately 10-15% of people with MS. PPMS is characterised by a progressive worsening of symptoms and disability right from the beginning, without periods of recovery or remission.
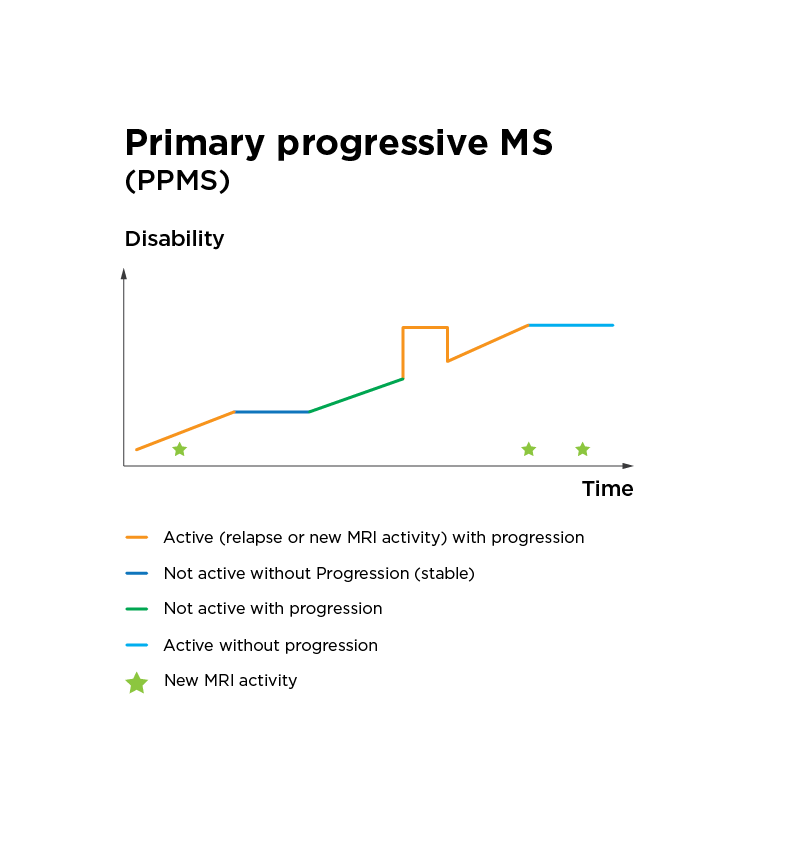
Anyone may develop MS but there are some patterns. Three out of four Australians with MS are women and the average age of diagnosis is just 30.
Studies suggest that genetic factors make certain individuals more susceptible than others, but there is no evidence that MS is directly inherited.
It occurs more commonly among people with northern European ancestry. People of African, Asian, and Hispanic backgrounds are also diagnosed with MS, however, the incidence is much lower. MS is not contagious.
In early MS, symptoms that might indicate any number of possible disorders come and go. Some people have symptoms that are very difficult for physicians to interpret, and these people must “wait and see.” While no single laboratory test is yet available to prove or rule out MS, magnetic resonance imaging (MRI) is a great help in reaching a definitive diagnosis.
Diagnosis is made by a neurologist who will work in partnership with your GP to determine treatment options and symptoms management. As early MS is not always easily detectable, it’s important you talk to a medical professional if you are displaying any of the symptoms of MS.
Understanding MS: An Introductory Guide
This guide was developed in collaboration with MS health professionals and in partnership with people living with MS.
This guide aims to:
- Provide reliable introductory information about multiple sclerosis
- Increase your understanding of various treatment and therapeutic strategies that will enable you to proactively collaborate with your healthcare team
- Assist you to understand the brain health perspective on MS and how you can embrace a brain healthy lifestyle
- Share where you can access trusted information, research, support and advice, now and into the future of your MS journey.
Download Guide